Dear Congress,
My father died last September. He was 68. He experienced severe, debilitating pain from his early teenage years until his death. I now experience similar pain from the same disease he had, Ankylosing Spondylitis (AS), and I fear daily that my life will follow the same path his did.
My dad looked like this (below) because he did not have access from a young age to effective treatments to slow down the progression of his disease:
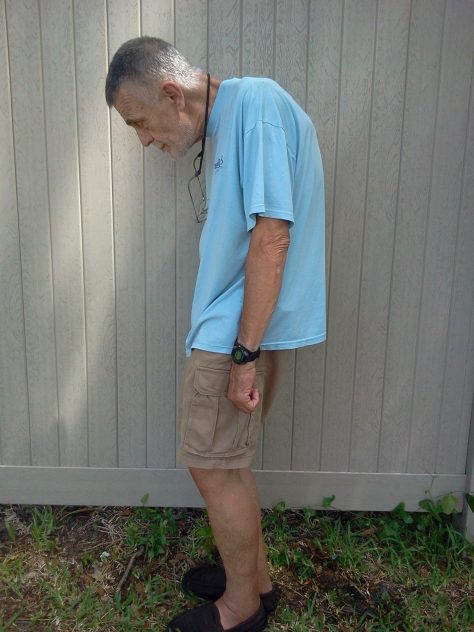
He didn’t have access to the treatments because they didn’t exist until 2003, when the first biologic drug was approved for treating patients with AS. By that time he was already a 90-degree hunchback, his spine fused in a rigid column of bone from knobby, painful bone spurs – he was slowly suffocating. The only thing a biologic drug could do was prolong his life and perhaps reduce some of the symptoms.
He died after two surgeries meant to straighten his spine, relieve his organs from being crushed, and give him a more horizontal line of sight. He’d been looking straight down at the ground for decades, unable to see in front of him unless he pivoted his body backwards with one foot pushed toe-first into the ground.
I learned I had AS in 2013 after a period of sudden, un-treatable illnesses that left me in pain and unable to breathe. Urgent Care doctors blamed my frequent visits on panic attacks and attempted to send me on my way with anxiety medication, but I knew my body better than that. Continue reading An Open Letter to Congress from a Poor, Disabled American





